Health
Low rates of access and insurance
Barriers to care
Treatment preferences
Traditional views of health, disease and healing
Women and childbirth
Additional concerns: crowding, depression, alcoholism, HIV/AIDS, teen pregnancy, domestic violence
Provider perspectives
Some innovative approaches
Low rates of access and insurance
Indigenous farmworkers are at a severe disadvantage when it comes to obtaining health care in California. They access care at rates far below the general population and decidedly lower than other Mexican-origin farmworkers.
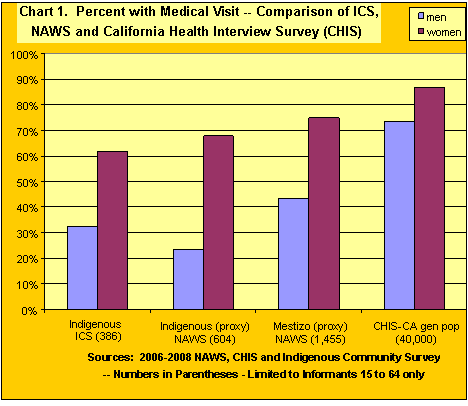
First, we focus on the women who, similar to all groups, obtain care at higher rates than men. In Chart 1 we show by two different measures (the National Agricultural Workers Survey-NAWS- and the Indigenous Community Survey-ICS) that indigenous women go to the doctor less than mestizo Mexican women. By one measure, 62% of the indigenous women and by another measure 68% of them have seen a doctor in the last two years. This compares to the much higher rate of 75% among the mestizo Mexican farmworker women. Now, if we look at the general population of women in the California Health Interview Survey (CHIS), we find that an even higher rate of 86% of women have seen a doctor. Next, if we look at men, we see much lower rates of visiting the doctor. Our two measures (NAWS and ICS) for indigenous men show that only 24% or 33% had medical visits while the 43% of mestizo farmworker males had seen a doctor. Not surprisingly, for the general population in California the rate for men of 73% is much higher than for any farmworker group (see Chart 1).
 Triqui men from Oaxaca in Greenfield, California. Indigenous men are particularly averse to medical care in California. Should they become ill, they self-medicate, seek care from traditional healers or return to Mexico. As a last resort they may go to an emergency room.Copyright David Bacon
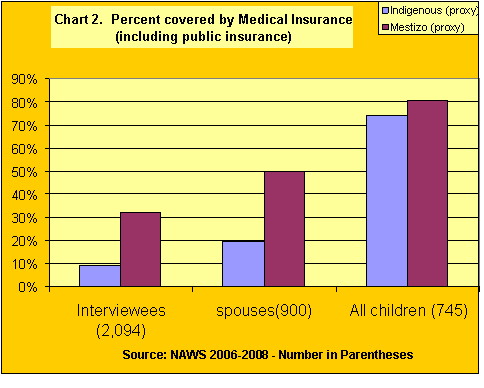
Triqui men from Oaxaca in Greenfield, California. Indigenous men are particularly averse to medical care in California. Should they become ill, they self-medicate, seek care from traditional healers or return to Mexico. As a last resort they may go to an emergency room.Copyright David BaconMoreover, insurance coverage for indigenous adults is extremely low, even when compared to the already-low rates for mestizo farmworkers. Only 9% of indigenous Mexican interviewees were covered and 19% of their spouses. The proportions for the mestizo farmworkers were much higher--31% for the interviewees and 50% for the spouses (see Chart 2). Indigenous children, however, are more likely to have coverage (over three fourths have insurance), since most were born in the U.S. and, given they are likely to be below the poverty line, they qualify for publicly-sponsored health care.
 A Mixtec woman and girl from San Martin Peras in the Mexican state of Oaxaca. They share a two-bedroom apartment with ten other family members on the outskirts of Watsonville where many Mixtecs work in the strawberry fields.
Copyright David Bacon
A Mixtec woman and girl from San Martin Peras in the Mexican state of Oaxaca. They share a two-bedroom apartment with ten other family members on the outskirts of Watsonville where many Mixtecs work in the strawberry fields.
Copyright David BaconBesides the cost of care and the lack of insurance, there are additional factors built into the system, together with cultural issues limiting access to health care. The systemic obstacles are well-known to those who study farmworkers and include: lack of transportation, inconvenient clinic hours, long waits, rude treatment by receptionists and staff, and fear related to immigration status. For the indigenous, however, there are additional linguistic and cultural barriers that impede obtaining health care in California.
Cultural-linguistic barriers
While hospitals are required by law to provide care in a language the patient can understand, compliance with this requirement is highly uneven. Frequently providers rely on the patient to bring in a friend or relative to translate, sometimes even a child, which raises difficulties when dealing with delicate matters and can result in misunderstandings. Others turn to telephone-based translation services with mixed results. The inability to communicate breeds distrust, avoidance of seeking care and non-compliance with prescribed treatments. As a Mixteco woman in Fresno put it, “I don’t think they prescribe the right medicine for what we have because they don’t understand what we’re saying.”
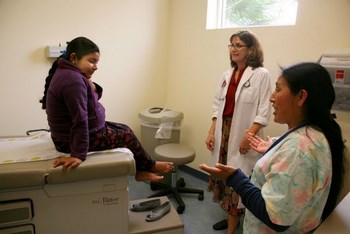 The Las Islas Clinic in Oxnard has hired native indigenous speakers to serve as interpreters. In some cases these interpreters are also trained as health outreach workers who are able to go out into the community to provide information and education on health matters. These health workers serve an extremely valuable function as cultural intermediaries. Pictured with patient are Sandy Young, Family Nurse Practitioner, and Sabina Cruz, Mixtec interpreter. Copyright David Bacon
The Las Islas Clinic in Oxnard has hired native indigenous speakers to serve as interpreters. In some cases these interpreters are also trained as health outreach workers who are able to go out into the community to provide information and education on health matters. These health workers serve an extremely valuable function as cultural intermediaries. Pictured with patient are Sandy Young, Family Nurse Practitioner, and Sabina Cruz, Mixtec interpreter. Copyright David Bacon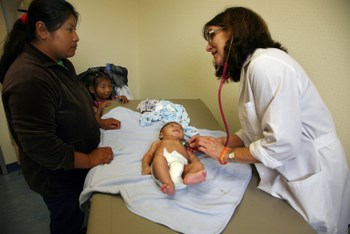 The Las Islas Clinic in Oxnard provides interpreters and culturally-competent care for its Mixtec patients. In so doing indigenous women are made to feel more comfortable seeking care for themselves and their children. Family Nurse Practitioner Sandy Young conducts a well-baby exam.Copyright David Bacon
The Las Islas Clinic in Oxnard provides interpreters and culturally-competent care for its Mixtec patients. In so doing indigenous women are made to feel more comfortable seeking care for themselves and their children. Family Nurse Practitioner Sandy Young conducts a well-baby exam.Copyright David BaconOver the last ten years or so, a number of clinics have recognized the need for indigenous interpreters and some have made the effort to reach out and hire indigenous speakers to work alongside clinicians. Providers on the Central Coast, and in the Ventura area in particular, are in the forefront of hiring indigenous interpreters to work on site, and some are able to provide culturally-competent care. To date, it is mostly Mixteco speakers who have been hired; as yet few services exist for Zapoteco and Triqui speakers.
Nonetheless, even when the interpreter is skilled, it adds extra time and cost, placing additional burdens on clinics that are already strapped for resources. In Oxnard, one highly accomplished interpreter who is trilingual in English, Spanish and her native Mixteco explained that there no words in Mixteco for numerous medical conditions such as asthma, tuberculosis, anemia and diabetes. As for women’s health, there are often no terms for certain body parts, particularly those relating to the reproductive system, or for procedures such as, for example, a cervical examination. Furthermore, indigenous women are extremely reticent to discuss matters related to sexuality and reproduction, particularly with male providers. Interpreters must employ patience, extra time and considerable tact to put women at ease and establish trust. They must also improvise language to explain unfamiliar concepts and procedures. The communication gap is hardly surprising given that many of the indigenous in California come from remote areas of Mexico with poor or non-existent medical services, and women in particular have had little prior experience with modern medical care.In hundreds of interviews, our research team repeatedly found people who were averse to the way U.S. medicine is practiced and sought caught care only as a last resort, often in the emergency room. They expressed mistrust in the providers and were often confused or angered by the treatment they received. As seen from the data in Chart 1 above, men in particular avoid seeking care, even when they have worked here for years. In the Central Valley, a community advocate explained that agencies frequently view the indigenous as “low-status” and make no effort to provide culturally-competent services. In the Salinas Valley, a Triqui lettuce-picker told us he doesn’t even bother trying to seek care because, as he put it, “They treat us worse than dogs.”
Care in Mexico
To avoid care by medical providers in the U.S., many indigenous reported that they go to Mexico. Medical services by for-profit providers in Tijuana cost a fraction of what they do in California, they require no confusing paperwork, and offer immediate attention. Drugs are also cheaper and available without a prescription. Many entrust relatives or friends to purchase their medicines in Mexico and then proceed to self-medicate. In spite of the extra effort, time and risk involved in traveling to Mexico, men in particular rely on the cross-border option. As a 36-year old Triqui farmworker in the Salinas Valley put it, “When they get seriously ill, they go to Mexico and afterwards they brave the border to get back. Few use the medical services here.”
Traditional healers
Another alternative is to seek the services of a traditional healer. Throughout California there are Mexican traditional healers discretely practicing their healing arts. They can be yerberos (herbalists), sobadores (massage specialists), hueseros (manipulators similar to chiropractors), curanderos (spiritual healers), or some combination thereof. Just about everywhere we conducted interviews people spoke of knowing traditional healers and of seeking them out for a variety of ailments. The treatments they receive are familiar and non-threatening; they are cheaper and perceived to result in positive outcomes. In a suburban house, in a quiet neighborhood on the Central Coast, we learned of one sobador who attended patients from seven in the morning until seven in the evening, charging on a sliding scale: five, ten or fifteen dollars, whatever the patient could afford.
With traditional healers in high demand, people lament the shortage of this kind of care as well as frustration at not having access to familiar medicinal plants or to traditional treatments such as a sweat bath (baño de vapor). Besides the therapeutic value of the heat and medical herbs, sweat baths play an important role in re-establishing a spiritual connection to the earth, a connection deemed essential for health. Women in particular miss having access to sweat baths following childbirth, as discussed in the section below.
Coping with illness
With the high cost of health care in California, the lack of insurance, the multiple barriers, and preference for care in Mexico or from a traditional healer, the indigenous tend to seek biomedical care only as a last resort. Going to a doctor in the early stages of a problem is likely to require a series tests which the indigenous view as an expensive waste of time. Those who have already been to see a doctor in Mexico prefer the quick diagnosis and prescriptions they receive without the need of “a bunch of machines.” And since prescriptions often involve antibiotics, some prefer to skip the doctor visit and move straight to self-medication. Antibiotics can be had at local flea markets or from someone who purchased them in Tijuana. Injections are prized as a quick way to get results and many people are able to inject themselves or know someone who can do the injecting.
Following are the steps people follow when coping with illness, as described to our researchers:
- Start with a traditional tea or home remedy, based on prior knowledge or the advice of relatives or neighbors. Failing that, and if one is available, seek advice from a salesperson at a Botánica, a store selling herbs and traditional remedies.
- Next, seek out familiar Mexican medicines used in the past, available at Mexican grocery stores or flea markets. People might ask for a particular medicine by name or describe symptoms to a store clerk and request a recommendation. Shopkeepers and flea market vendors become their de facto pharmacists.
- If these efforts fail to provide relief, next visit a Western-style drug store to purchase over-the-counter medications recommended by a friend, neighbor or relative.
- If a traditional healer is available, the person may seek treatment in exchange for a small fee.
- Finally, if seeking treatment in Mexico is not an option, and after all avenues have been exhausted and the condition has worsened, the person will reluctantly go to the clinic or emergency room.
Traditional views of health, disease and healing
Gaining a sense of an indigenous person’s belief system and worldview can help us understand why indigenous patients avoid modern medical care, and why they often do not comply with the prescribed treatment. Within many traditional societies a person’s relationship to nature, the community, the spirit world and the cosmos all play important roles in one’s health and wellbeing. An essential feature is the importance of maintaining equilibrium between all the forces at work in the world. One of the most frequently expressed needs, in Mexican indigenous societies as well as others, is the need for balance between “hot” and “cold,” concepts that do not necessarily relate to temperature. Below is an excerpt from a discussion of the hot-cold duality concept by a renowned Mexican scholar, Federico Navarrete Linares (the translation is ours):
“Nearly all indigenous peoples believe that the world has elements, or forces, that are either hot or cold. Hot elements are associated with the sun, the sky, the masculine, order, light and life. Cold elements are associated with the moon, the earth, the feminine, disorder, darkness and death. Although hot elements are considered superior to cold elements, it does not follow that the former are good and the latter bad, since both are necessary for life. Plant growth, for example, requires the heat and light of the sun, but also depends on the cold forces of earth and death [decomposition]. While males possess a greater quantity of hot elements, they also require cold elements to maintain health; women in the same way need hot elements. Similarly, there are hot diseases that cause an excess of heat in the body, and cold diseases that lead to excessive temperature loss. What’s important, according to the indigenous worldview, is the balance between these opposing forces. Equilibrium is necessary for human health, for social tranquility and wellbeing, and it’s important in the wider sense as well, to ensure that plants grow and life continues.”
Indigenous healing practices, Navarrete tells us, depend on an intimate knowledge of the environment and of local plants and animals. The healer makes use of his or her knowledge of the pharmaceutical properties of plants, as well as knowing their hot and cold attributes.
When a Mixteco woman who works as a medical interpreter in Fresno was asked about the hot-cold concept of illness causation, she explained, “When it’s cold you need to avoid ‘cold’ foods such as rice. When it’s hot you should avoid foods such as mango.” When she was asked if medical personnel in the local hospital were aware of these sorts of things, she relied that they simply don’t discuss this with the doctor.
- For further discussion of indigenous views of health, disease and healing, see Section VIII-3 of the IFS Report.
- The quote from Federico Navarrete Linares can be found in Los pueblos indígenas de México. México: Comisión Nacional para el Desarrollo de los Pueblos Indígenas, 2008, pp. 78-79. http://www.cdi.gob.mx
- The medical anthropologist Bonnie Bade offers valuable insights into contemporary Mixteco medicine (see Bibliography in IFS Report).
Care related to childbirth and delivery may account for the majority of encounters between the indigenous farmworkers and the health care system. Yet indigenous women view clinics and hospitals with fear and often delay seeking care until they are going into labor. Our informants gave a variety of reasons why women avoid prenatal care: the indigenous women are not accustomed to prenatal care at home in Oaxaca; they could not get to a clinic; they did not want to lose a day’s work; they disliked the impersonal treatment and the use of machines and tests; they did not trust providers to address their concerns; and, they have a profound fear of being given a Cesarean section.
The contrast between the indigenous and biomedical approaches to childbirth is like heaven and earth according to one Mixteco health outreach worker in Fresno. She explained that indigenous women traditionally think of pregnancy and childbirth as a happy time, pre- and post-partum practices include hot herbal teas and massages. But here, she said, its all about machines. Of course theyre going to be alarmed! She went on to describe how upsetting the women find blood tests, ultra-sound, and the bright lights and high-tech environment of the delivery room where they are surrounded by people they dont know, speaking a language they dont comprehend. And, in cases of Cesarean deliveries, they dont understand why the procedure is necessary and believe it is due to the doctors incompetence. Finally, following childbirth, Mixteco women in their home communities are used to a carefully-prescribed regimen of sweat baths taken under the supervision of older, experienced women. The baths include the use of medicinal herbs to aid recovery and help re-establish the bodys equilibrium. The lack of sweat baths can contribute to the profound sense of isolation and post-partum depression that indigenous women experience on this side of the border.
For a first-hand account of a Mixteco sweat-bath experience, see “Alive and Well: Generating Alternatives to Biomedical Heath Care by Mixteco Migrant Families in California” by Bonnie Bade in Indigenous Mexican Migrants in the United States, Jonathan Fox and Gaspar Rivera-Salgado, editors. La Jolla: Center for U.S.-Mexican Studies and the Center for Comparative Immigration Studies, University of California, San Diego, 2004.
Another cultural disconnect exists in the area of maternal nutrition during pregnancy. Providers report that many indigenous women are anemic and will prescribe vitamins. Indigenous women, for their part, are reluctant to take the vitamins, fearing they will cause their baby to grow too large, putting them at risk for a C-section.
The fact that indigenous women do not recognize the gynecological and obstetric care they receive in California is safer and likely to result in better outcomes than giving birth in Mexico only underscores the deep cultural divide that exists between themselves and U.S. providers. (By some estimates, an indigenous woman is nearly ten times more likely to die in childbirth in Mexico than she is in the United States-- see page 82 of the IFS Report.)
When providers strive to find culturally-appropriate ways to care for indigenous women, the results are promising. In Ventura County several of the clinics have hired Mixteco interpreters to improve communication and provide a welcoming environment. In Oxnard, a Family Nurse Practitioner, who sees many Mixteco patients, can demonstrate (based on data from her practice) that culturally-appropriate care does lead to earlier dates of entry into prenatal care for pregnant Mixteco women. Other efforts to reach out to the indigenous population are described in “Innovative Approaches” below.Additional concerns: crowding, depression, alcoholism, HIV/AIDS, teen pregnancy, domestic violence
We have no data on the frequency of given health conditions, specific diseases or outcomes since no data is kept for Mexican minority language groups by county health departments. What follows is drawn from interviews with key informants, including providers, community activists, members of the indigenous communities, as well as from field observations by our research team.
Crowding
In the Housing section we described the extraordinarily high rate of crowding among indigenous farmworkers. Providers expressed grave concern over the health implications of these poor housing conditions, including: a greater risk of respiratory infections (including tuberculosis) among people living in such close quarters; a greater risk for the rapid spread of epidemics in this largely non-immunized population; poor nutrition due to lack of food storage and cooking facilities; lead contamination in small children; poor hygiene; delayed child development; domestic violence.
Depression
Our researchers learned that depression afflicts both men and women who find themselves culturally and linguistically isolated and far from home and their extended families. Again, there is no administrative data and consequently little attention paid to issues of mental health. However, this is viewed by informants as an area in urgent need of attention.
Among indigenous women informants report that post-partum depression is a serious condition that has resulted in suicide in some cases. Many are very young women, often in their teens, who are away from their homes and villages for the first time in their lives. Moreover, transportation is limited and they have no access to the traditional healing rituals during this time of heightened physical and emotional vulnerability.
Since indigenous men seldom approach clinics for help, the following observations come from community outreach workers. They described an unhealthy syndrome that develops among men living on their own, be it in encampments, in crowded apartments, in garages or sheds. The men miss their families, have unhealthy diets, lack opportunities for recreation and exercise, and often fall prey to alcohol and drug use. These conditions deteriorate their physical and mental health. One Mixteco outreach worker described men he saw living in the canyons of San Diego as profoundly sad and overcome with feelings of inferiority and impotence. An outreach worker in northern California explained why the newly-arrived indigenous men find it hard to adapt. First, they are frustrated by daily experiences of exploitation by foremen, merchants and landlords. Moreover, they have little news of their families back home. When they fail to achieve the goals they had set for themselves, their stress levels go up, and this often drives them into depression. Many spiral into alcoholism. Another condition that has received little attention is what outreach workers believe could be Post Traumatic Stress Disorder (PTSD), resulting from the violence and abuse they experience while crossing the border.
Alcoholism
Community workers throughout California report that alcohol consumption and binge drinking are resulting in multiple problems for the indigenous community, including driving while intoxicated, domestic abuse and high-risk sexual behavior.
HIV/AIDS
Again, while we have no data on the rates of HIV/AIDS infection in the indigenous community, informants report that there is considerable fear and misinformation regarding the disease coupled with a strong resistance to the use of condoms. Outreach workers in the Central Valley described indigenous men who are under the impression that contact with pesticides can lead to HIV/AIDS. Others believed they could protect themselves by rubbing their penis with lemon following sexual relations. Even those who were diagnosed HIV-positive described using bleach on their penises. Efforts to encourage protective behavior have proved frustrating.
Teen pregnancy
Early age of marriage and childbearing is deemed culturally acceptable within the indigenous community, and in Oaxacan villages it is not unusual for girls to give birth to their first child at age fourteen or fifteen. We compared the age of the mother at the birth of the first child for the indigenous women in our study to this age for women in general in California. As shown in Chart 3, more than half of the indigenous women (57%) have their first child before they have reached the age of 20. Compared to women in the general population in California, only 25% have their first child when they are less than 20. In other words, more than twice as many indigenous women give birth when they are still under 20 than the general population of women in California.
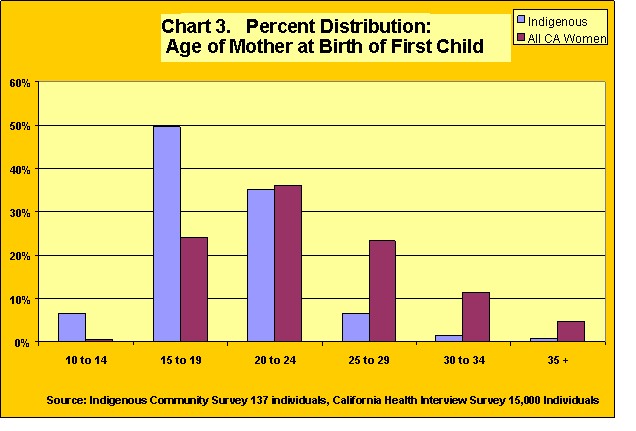
This early age of childbearing raises concerns for medical providers. They report that it can lead to premature births, low birth weights, endanger the young mother’s health, and increase their risk for malnutrition, high blood pressure and anemia.
Teen pregnancy also raises other concerns in the context of U.S. norms, institutions and laws. In cases where the girl is an unaccompanied minor and the partner/father is several years older than the girl, the father can be charged with statutory rape and imprisoned. This can leave the young girl alone and frightened in a strange country, with a new baby, unable to speak English or Spanish, and without means of support.
Domestic violence
Outreach workers and health providers consider this a serious problem that is extremely difficult to identify and resolve. At present, informants report that little is being done to confront the issue. It is a problem whose roots lie deep within indigenous communities and Mexican society where women have traditionally had few rights and where violence against women has been accepted as “the cross women must bear.” Again, we have no data on the prevalence of domestic violence within the indigenous community, but it is clear that it exists within indigenous households in California and it is causing considerable pain and suffering.
Paramount among the barriers to addressing this problem is the lack of a culturally-appropriate strategy. Whereas health workers describe repeatedly encountering cases of women who are victims of abuse by their partners, they nevertheless find the women unwilling to press charges against their abusers. This reluctance emerges from the well-grounded fear of being ostracized by both their families and their community. The few women who have taken the bold step of leaving their abusers and moving into a shelter have found themselves in an even worse predicament when their time was up at the shelter. They discovered that their community had rejected them, and since they are unable to speak English, and only limited Spanish, they simply had no place to go.
One group on the Central Coast has organized informational meetings for the local indigenous community to address a range of topics, including sexual assault and domestic violence. The activist spearheading the group reports that while meetings have been well-attended, there are many in the community who shun the meetings out of fear that their women will become “uppity.” At present, providers and activists wishing to help indigenous women are constrained by the lack of appropriate counseling services, the lack of safe housing for those wishing to escape their abusers, and the inertia of a community that does not consider it a problem.Provider perspectives and challenges
The appearance of Mexican indigenous patients in significant numbers caught the health care system off guard and unprepared. Prior to the late 1990s few providers distinguished indigenous patients from other Mexican immigrants, or had any background knowledge or training in how to deliver culturally-appropriate care. A bilingual Spanish-English Family Nurse Practitioner at a community clinic in the Ventura area reported that she only became aware of this distinct group around 1998, when she began to see patients who spoke little or no Spanish. Ten years later half of her patients are Mixteco, and she and her colleagues have begun to see other indigenous groups including Zapotecos, Triquis and Amuzgos.
In addition to the language barrier, providers trained in modern bio-medical medicine note other challenges they face in trying to serve the indigenous. In particular, they described the difficulty of communicating with people who have very low levels of education, little or no exposure to western medicine and technology, and who hold entirely different notions of disease, its causation and treatment. Furthermore, indigenous women have limited knowledge of their own bodies and reproductive systems, have no vocabulary for many internal body parts, are extremely reticent about discussing matters of sex and reproduction, and are fearful of being touched by male providers. Indigenous men often insist on being present during the doctor visits, which interferes with doctor-patient confidentiality.
Many lament the lack of health materials suitable for a barely literate population. Of particular importance are materials on contraception, the risks associated with teenage childbearing, information on prenatal care, as well on post natal care and child safety, given the dramatic difference between conditions in remote villages and modern-day California.
Most providers and activists spoke of the urgent need for more interpreters. In some areas, particularly the Central Valley, clinic administrators have been slow to acknowledge the need for interpreters, in spite of the large indigenous presence. In other areas, along the Central Coast for example, administrators wanting to hire indigenous interpreters have found they cannot hire the best candidates because they lack legal papers.
Finally, providers report that it takes extra staff time to care for indigenous patients. This places additional demands on a public health care system that is already under stress due to a lack of family practitioners and limited resources.
In spite of the constraints and challenges, organizations and providers around the state are devising creative ways to deliver culturally-competent, quality care for the indigenous. Providers on the Central Coast, in particular Ventura County, have been developing new strategies to reach out to and serve the indigenous population. Additionally, several indigenous-run organizations have programs and services to improve the health and wellbeing of the indigenous population. Below, we list a few examples of these efforts (there are many others not listed here):
 At Las Islas Clinic in Oxnard Mixtec interpreter Sabina Cruz clarifies medical instructions for a patient. Copyright David Bacon
LikeUnlike
At Las Islas Clinic in Oxnard Mixtec interpreter Sabina Cruz clarifies medical instructions for a patient. Copyright David Bacon
LikeUnlike- A number of clinics and hospitals now have native indigenous speakers on staff to serve as interpreters. In some cases these interpreters are also trained as health outreach workers who are able to go out into the community to provide information and education on health matters. These interpreters/health workers serve an extremely valuable function of cultural intermediaries.
- A family clinic in Oxnard, working in collaboration with the OB/GYN department of the county hospital, organizes visits to the hospital for pregnant Mixteco women. With a Mixteco interpreter accompanying them, the expectant Mixteco mothers are shown the delivery room and alerted to what to expect. These visits represent an effort to help allay misunderstanding and fear.
- One clinic has begun screening pregnant women for depression. They have provided mental health counseling, using interpreters as intermediaries. The clinic’s administrator estimates that over the previous year they were successful at preventing at least ten suicides.
- The Mixteco/Indígena Organizing Project (MICOP) offers a number of important services to address the needs of the indigenous community in Ventura County. These include training interpreters to work in clinics and with local organizations as well as training health outreach workers (promotoras de salud ). Among their many activities are Well-Baby classes which provide an opportunity for addressing post-partum depression. In the classes small groups of Mixteco mothers meet with two outreach workers and are encouraged to express their feelings and share experiences. MICOP believes the group setting is a culturally appropriate way to provide support for women dealing with depression as well as the other challenges they face living in an unfamiliar environment. (For more information about MICOP see www.mixteco.org)
- CBDIO (Centro Binacional para el Desarrollo Indígena Oaxaqueño) is an indigenous-led organization with offices in Fresno, Santa Maria, Los Angeles and Oaxaca. It has been at the forefront developing programs to improve health and health care for the indigenous. It has trained interpreters, maintains a directory of translators, and provides interpretation services in Mixteco, Triqui, Chatino and other indigenous languages. It offers workshops for the indigenous community on health matters and it organizes conferences for the provider community to educate them about the indigenous community and its needs. Its local offices serve as cultural intermediaries, helping the indigenous navigate the U.S. health care system. These offices also help relieve the burden on local clinics by assisting patients with their medical and social services paperwork. (See: http://centrobinacional.org/)
- Radio Bilingue and a number of local stations provide programming in Mixteco, Triqui, Zapoteco and Chatino, frequently discussing health topics, diet, nutrition and informing their listeners about clinics with interpreters on staff.
- The Oaxacan Cultural Project in Hollister has organized health education workshops and invited a physician for presentations on women’s health in Spanish and provided translation into Triqui and Mixteco. The physician was able to address women’s concerns about C-sections and other matters related to the reproductive system.
- The Unidad Popular Benito Juárez (UPBJ) based in Bakersfield serves the indigenous community by organizing workshops, youth activities and various cultural events. It also hosts a lively listserve dialogue on historical and cultural issues related to the indigenous (see UPBJ.org).
- The University of California’s Health Initiative of the Americas (HIA) arranged for a traditional practitioner from Oaxaca to visit California during the 2008 Binational Health Week. The visiting practitioner spoke in Mixteco on Radio Bilingue and gave numerous talks and workshops around California, for the indigenous community as well as for health care professionals. Simultaneously HIA made available a booklet in English and Spanish titled Mesoamerican Traditional Medicine (a copy is available at http://hia.berkeley.edu/documents/medicina_tradicional.pdf)
Links to other organizations serving the indigenous can be found on our page of links.




